Clinical Excellence: The Science of Care
find the feature below, as well as other examples of what makes ysn a singular place for leadership & scholarship, in the latest edition of yale nursing matters magazine – now posted online.
“I was curious,” says Associate Professor of Nursing Jessica Coviello, DNP, APRN, ANP-BC. While caring for women with cardiovascular disease, she began to notice how many of them were coming in with heart failure several years after undergoing chemotherapy for breast cancer. She wondered if there was a connection.
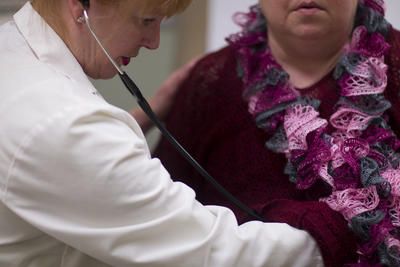 An Advanced Practice Registered Nurse, or APRN, like Coviello, is well-poised to delve into this question. As registered nurses with advanced degrees - a Master’s or a Doctorate - in nursing, “APRNs are not only clinicians,” she says, “but they really should be scholars as well.” Nursing research focuses on the science behind clinical practice, as well as prevention, and managing the symptoms related to a variety of illnesses. Clinically, APRNs can act as Nurse Practitioners (NPs), Certified Nurse Midwives (CNMs), Certified Registered Nurse Anesthetists, or Clinical Nurse Specialists. The Yale School of Nursing’s APRN programs for NPs and CNMs are top-ranked in the nation.
An Advanced Practice Registered Nurse, or APRN, like Coviello, is well-poised to delve into this question. As registered nurses with advanced degrees - a Master’s or a Doctorate - in nursing, “APRNs are not only clinicians,” she says, “but they really should be scholars as well.” Nursing research focuses on the science behind clinical practice, as well as prevention, and managing the symptoms related to a variety of illnesses. Clinically, APRNs can act as Nurse Practitioners (NPs), Certified Nurse Midwives (CNMs), Certified Registered Nurse Anesthetists, or Clinical Nurse Specialists. The Yale School of Nursing’s APRN programs for NPs and CNMs are top-ranked in the nation.
Spurred on by what she saw in her daily practice, Coviello began to investigate the cardiac consequences for breast cancer chemotherapy treatments, and what protocols were in place to prevent them. “I came to realize,” she says, “there was actually no guideline for patients to have a cardiovascular assessment before they received treatment.”
She was surprised at the omission. “It was pretty astounding to me that no one looked at cardiovascular risk before people received drugs that put them at risk.” Along with a colleague, Coviello set to work designing a study to examine cardiovascular risk in women with breast cancer. Their research uncovered that many women entered chemotherapy with several risk factors for heart disease, including hypertension, and high body mass index. “They were set up for metabolic syndrome,” she says. “Then during treatment, they received a drug, Decadron, which made that metabolic syndrome worse.”
Coviello’s experience is a powerful example of the clinical excellence achieved by APRNs: by looking at the whole health of her patients, rather than at just the particular ailments that brought them to the clinic, she was able find this gap in care. This holistic approach to patient care is a hallmark of the APRN.
While the practice of medicine has traditionally been founded upon curing disease, “nursing is a preventive model,” says Coviello. “Even looking back to Florence Nightingale’s work, she was looking at how you could create a healthy environment for individuals,” rather than just treating disease. In Coviello’s practice, “the gaps that we found were the gaps that were related to risk. If you don’t look at risk prevention, or if you don’t act on risk, then you end up with an ailment.”

Nursing draws from clinical, basic, social, and translational science to inform practice, and APRNs work squarely in the model of evidence-based care. The role of the APRN began in the 1960s as a response to the increased need for primary care, as Medicaid and Medicare coverage expanded. Similar urgency has been felt in recent years with the expansion of coverage seen with the Affordable Care Act (which recently withstood a Republican challenge for repeal). As the need for primary care has grown in the U.S., so has the contribution of APRNs to diagnosing, treating, managing, and preventing illness. Recently, the Veteran’s Health Administration ruled to grant APRNs nationwide full practice authority, including prescribing medications, and interpreting test results. While many APRNs practice in ambulatory settings, acute care NPs practice in hospitals to improve health outcomes for patients who receive sometimes overwhelming amounts of information from many providers.
“We are taught from day one to take care of the whole person, not just their medical condition,” says Elizabeth Doyle, DNP, APRN, PNP-BC, BC-ADM, CDE. Doyle is a Lecturer in the Pediatric Nurse Practitioner specialty, and conducts clinical research on diabetes.
“Diabetes care really lends itself to the care of an APRN,” Doyle says. “My colleagues and I have a saying about diabetes care: it’s 15 percent medical care, and 85 percent worrying about the rest of the patient’s life, and the psychosocial influence on their care.” In her practice, Doyle is investigating how to best transition adolescent diabetes patients from pediatric to adult care. Older adolescents, she observes, make for a challenging cohort of patients. “They don’t quite belong in pediatrics, because they are becoming more independent,” she says, “yet they still really need additional support, because they are not quite ready for the level of independence that is expected in an adult practice.”
As she worked with young adults, she began to notice a high incidence of a dangerous practice, disordered eating, in her patients, interestingly in both girls and boys. “Patients with diabetes learn if they skip insulin, they’ll lose a lot of calories in their urine, and they’ll use it as a form of weight loss. It becomes a type of purging. That’s pretty unique to diabetes.” The practice causes a threefold increase in mortality among diabetes patients, but, as Doyle discovered, “there are no guidelines on how to treat this.”
To address this gap, Doyle is collaborating with a psychologist and colleagues at the Yale Diabetes Center to help patients address their disordered eating habits with mindful eating. She is also working with Dr. Robin Whittemore, director of YSN’s PhD program, to develop a pilot study to examine the effectiveness of this type of treatment. “There isn’t really any research, other than anecdotal, on how to treat this.”
Both Doyle and Coviello are Doctors of Nursing Practice (DNP). As DNPs, “our job is to take the research, and operationalize it,” says Coviello. Often, “research sits there, and it takes too long for things to change. The process of bench to bedside can take almost 20 years. That’s why the DNP was developed, to help fill in that gap. We are leaders in taking evidence and turning it into practice.”
“All of the research I have been involved in has stemmed from practice,” says Dr. Doyle. “We are taught to utilize evidence, and go out to create the evidence if it doesn’t exist. We identify a problem, and if we don’t know how to care for patients with that problem, our goal becomes to find out how to care for them.”
The evidence-based care provided by APRNs is founded on outcomes proven by research. Evidence-based care refutes and replaces traditional types of care that relied merely on what had always just been done. “There are so many things that are traditional, what we call ‘sacred cows,’” says Associate Professor of Nursing Laura Andrews, PhD, APRN, ACNP-BC. “There are things that are written in stone and nobody knows why. They came down from the mount eons ago, but we still do them.”

Andrews specializes in acute and critical care. “One of the standard norms in acute care is the temporary feeding tube, used in feeding liquid nutrition. The custom is that you aspirate back on it, and see if there is a residual, and that’s how you can tell if a patient is tolerating the tube feeds or not,” she says. However, she has found, through evidence that comes from practice and research, that this practice actually harms the patients. “Critically ill patients need nutrition, and if we keep checking residuals and stopping feeding, patients never meet their nutrition goals.”
A major challenge that APRNs face in operationalizing these evidence-based findings, Andrews says, is a culture of habit, which is slow and difficult to change. “Some of these traditions are hard to get through,” she says. “Despite having all this evidence that it’s actually harmful, it’s so engrained in people’s practice.”
Because of extensive experience working as part of a team, and expertly coordinating between physicians, residents, nurses, and other staff, APRNs are able to lead this charge for change. At the Hospital of Central Connecticut’s New Britain Campus, where Dr. Andrews cares for patients, she is working to implement a policy to change the feeding tube practice, but it is still commonly done. To reduce the practice, she is training medical residents, nurses, and physicians assistants on its dangers, and educating them on how to change it.
When change does happen, it is powerful. Dr. Coviello was able to operationalize the results of her research, and collaborated with two cardiologists to begin a cardio-oncology clinic at Smilow Cancer Hospital. The clinic assesses patients who are about to begin chemotherapy for cardiovascular risk, and now sees up to 50 patients per week, though Coviello would like to see every patient prior to chemotherapy to assess them for risk. “Our primary job at Smilow is to keep people safe through their treatments,” she says. This goes beyond reducing cardiovascular risk. “If patients need dietary care, I refer them. It’s always with this holistic idea, trying to create an interdisciplinary team for patients.”
The APRN’s holistic approach to care not only identifies protocols and clinical needs that might fall through the cracks, but can provide a safety net for vulnerable groups of patients, who might fall through the cracks themselves. Erin McMahon, CNM, EdD, is a nurse midwife at the Vidone Birth Center at Yale New Haven Hospital’s Saint Raphael Campus. “Vulnerable women can really benefit from a midwife who is not only talking to her about her pregnancy, but will also say, what else is happening at home?” says McMahon. “We are trained to look at what else is going on in a patient’s life that we know will impact a person’s pregnancy; such as adequate food, or safety.”

One recent patient returned to the hospital shortly after giving birth, along with her children. “She told us she didn’t feel safe at home,” Dr. McMahon recalls. “She knew, because she had been with us before, the birth center was a safe place, and if I go there, they will help me.” Once patients confide in them, APRNs must then know whom to reach out to in the community to get patients the help they need. “We couldn’t provide housing, we didn’t have a safe place for her to go, but we had a social worker on our team who could connect her to the necessary resources. We provided lunch for her and her children while the team worked on a safe plan. And she then went from our clinic to a private, secure shelter that day,”
Patricia Ryan-Krause, MS, MSN, RN, CPNP, cares for refugees at Yale’s outpatient Pediatric Primary Care Center, where New Haven’s local agency for helping immigrants and refugees, IRIS, brings people who have recently arrived in the city for their initial comprehensive health care visits. Refugee patients “have had a total disruption in their life and their family,” says Ryan-Krause. Because there is so much ground to cover in these visits with refugee patients, it is “essential to go beyond the checklist of a routine visit,” says Ryan-Krause. “For clinical excellence, it’s important to engage the family. It’s based on responding to the family’s needs, and doing so in a culturally sensitive way.”
Part of this sensitivity means not having any assumptions about what new arrivals might expect from their health care providers. Children, in particular, are at risk for mental health, behavioral, and developmental issues upon arriving in the U.S. The challenge for their caregivers, says Ryan-Krause, is that many of their home cultures do not recognize these issues. “We expect people to know what well care is,” or to understand the importance of evaluating development in children, she relates. “In Syria, if a child is sick, they try home remedies, and if they don’t work, they go the pharmacy where they can buy anything, from controlled substances to cough drops, and then they might go to the doctor. But there are no wellness visits to talk about nutrition, safety, or development. We need to talk about what these visits mean.”
 The APRN delivering care to refugee families must recognize their courage and resilience, and that “every person from the same country does not have the same culture, or experience things in the same way,” she says. “All that being said, we still need to address issues of health promotion and health safety when we are taking care of these families.” For example, she sees many patients who, as part of an ancient tradition, use kohl, a black eyeliner, on small children to protect their eyes. Kohl is full of lead. “We always suggest that there are other products,” she says, “but you have to be sensitive to their culture, and listen to the concerns of the family.”
The APRN delivering care to refugee families must recognize their courage and resilience, and that “every person from the same country does not have the same culture, or experience things in the same way,” she says. “All that being said, we still need to address issues of health promotion and health safety when we are taking care of these families.” For example, she sees many patients who, as part of an ancient tradition, use kohl, a black eyeliner, on small children to protect their eyes. Kohl is full of lead. “We always suggest that there are other products,” she says, “but you have to be sensitive to their culture, and listen to the concerns of the family.”
“To me, clinical excellence is caring for the patient, and caring for the whole family,” says Nancy Banasiak, MSN, PPCNP-BC, APRN. Banasiak works with patients with asthma, and a large part of her role, she says, is making sure that her patients, often from underserved, low-income communities, have the medications they need to manage their asthma, and keep them from going to the emergency room with acute asthma exacerbations. “There are ways to find medications, but maybe parents don’t have time, or knowledge, or access to the internet,” she says, and it is up to the APRN to help them navigate the challenges of the health care system. “I think that is one piece missing in health care today, the notion of advocating for patients.”
In acting as advocates for patients, “one of the things that midwives and nurses do is offer respect,” McMahon says. “Some women are not getting that in their life, especially if they are trying to use a federal system to access safety net services, housing, or food stamps. Sometimes, we don’t always treat people very well. The idea that somebody would sit down and say, ‘So tell me how you would like this birth to go? How can we get you enrolled in school? How can we get you child care so you can attend classes?’ - that adds value.”

McMahon underscores that holistic care means treating patients as individuals. The Vidone is a midwifery-led unit, in which the focus is on natural physiologic birth, guided by the conviction that most of the time, labor and birth progress normally. The midwife monitors labor, and decides when intervention is necessary, including transfer to obstetrician and surgical delivery, if needed. “The best care for women is when we work together, and we negotiate,” she says. “Looking at each individual woman, and saying, what does the evidence say we should do to assist her with her pregnancy or her labor?”
As an academic clinical center, the Vidone exposes health care providers to a wide array of complications. “When you have seen really sick moms and babies, you can start to see disaster looming around every corner, but our role is to help everyone remember that not all women are those women,” she says. “Midwifery care is about the judicious use of interventions, to make sure we are not just applying them to everybody, but that we are applying them in an evidence-based way.”
Sometimes, examination into long-held practices reveals surprising insights. Since the 1970s, electronic fetal monitoring, which essentially allows a labor team a window into the womb, with constant information on contractions and fetal heart rate, has been a delivery room staple. “You would think if we listen in all the time, that the outcomes are going to be better,” McMahon says.
The evidence, however, proved otherwise. Research revealed that “constant monitoring did not change rates of cerebral palsy, or complications related to birth,” she says. “What it did do was increase Caesarean section rates, without necessarily improving outcomes for the moms and babies.” Increasing Caesarean rates, which have been on the rise for the past several years, is responsible for many complications for the mother after birth, including placental problems, and hysterectomies after multiple Caesarean deliveries. “What the evidence has shown us is that for a normal, low-risk labor, intermittent monitoring is just as protective, and our outcomes are just as good.” That is now the practice at the Vidone for low risk women.
APRNs are constantly making connections: between physician and nurse; researcher and clinician; patient and community. At heart, APRNs are clinicians, collaborators, investigators, and teachers, and could not fulfill one of those roles without full commitment to the others. “The best teachers were those who stayed in clinical practice,” says Jessica Coviello, “because each of those worlds informs the others.”
 “I think we are in a good position,” says Laura Andrews, “because we provide quality care to patients, and we are training the next generation.” This education is based on a deep experience of caring for patients. “Because I work clinically, I am a better educator, and because I work in academics, I am a better clinician,” she says. In health care, “everything changes so quickly. If I am not firmly rooted in clinical care, what am I teaching my students?”
“I think we are in a good position,” says Laura Andrews, “because we provide quality care to patients, and we are training the next generation.” This education is based on a deep experience of caring for patients. “Because I work clinically, I am a better educator, and because I work in academics, I am a better clinician,” she says. In health care, “everything changes so quickly. If I am not firmly rooted in clinical care, what am I teaching my students?”
All of it, for the APRN, is driven by one thing: caring for people. Being in the clinic with patients “feeds my soul, and it makes me a better teacher, says Coviello. “Those of us who do it, we do it because we love it.”
