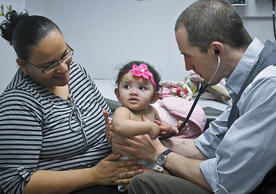
Filling Critical Gaps in Primary Healthcare: Advanced Practice Registered Nurses Meeting the Challenge
By Katherine L. Kraines
For many health care providers, meeting the needs of patients is a daily if not an hourly challenge. Increasing regulation, a plethora of new technologies and information, an aging population, the needs of the disenfranchised, and greater consumer expectations and awareness exert unrelenting demands at every level of care. All of this is further complicated by a shortage of physicians, particularly in primary care. 55 million Americans live in areas with a shortage of primary care providers.
Over the past fifty years, the role of advanced practice registered nurses (APRNs), which includes nurse practitioners (NPs), has evolved to increasingly meet patient needs in both the inpatient and outpatient settings. APRNs are registered nurses educated at a master’s or post-master’s level for a specific clinical role and patient population, with certification reflecting the specialized nature of the graduate program.
Currently, there are about 234,000 licensed APRNs in the United States, and nearly 87 percent are certified in an area of primary care. The four types of APRNs include the nurse practitioner (NP), nurse anesthetist (CRNA), clinical nurse specialist (CNS), and nurse midwife (CNM). Under the NP umbrella are specialties in adult/gerontology acute care and primary care, family care, pediatric care, and psychiatric care.
According to Philip Martinez, EdD, MSN, APRN-BC, director of the Yale School of Nursing (YSN) Graduate Entry Prespecialty in Nursing program, a YSN graduate and full-time acute care nurse practitioner, APRNs can assess patients, order and interpret diagnostic tests, make diagnoses, prescribe medications, and initiate and manage treatment plans across a spectrum of settings and specialties. All APRNs consult and collaborate with their physician colleagues, and many of them practice as part of a healthcare team. For example, Martinez is a member of the pulmonary intensivist team for a 12-bed ICU where patients are seen by a multidisciplinary team that can include other APRNs, physicians, nurses, dieticians, pharmacists, clergy, and social workers.

“The APRN movement started in the 1960s, and YSN was a huge innovator in nursing practice, developing the first graduate level nurse practitioner program in the U.S. in 1969,” said Carmen Portillo, R.N., Ph.D., FAAN, YSN executive deputy dean, and professor. “Our focus continues to be a program that graduates the very best APRNs in the country.” YSN master’s students can specialize in one of six areas: adult/gerontology acute care, adult/gerontology primary care, family nurse practitioner, nurse-midwifery/women’s health, pediatrics, and psychiatric-mental health. Highlighting the need for more providers in primary care, Portillo said that “APRNs fill a critical slot and there is a tremendous need for more APRNs in acute care, primary care and psych-mental health.”
APRNs are ready to see more patients and ease some of the stresses on the healthcare system, particularly to underserved populations in rural and urban settings. But barriers continue to inhibit their ability to practice to the full extent of their training, education, and certification. While several agencies license APRNs based on their specialty, each state has a board of nursing that determines the APRN scope of practice and can put different restrictions in place. Martinez said the most significant restriction is that not every state allows APRNs to practice independently. He stressed that it is a misconception to think that independent means without others; rather, “It means that APRNs are the ones patients come to first, and then we collaborate with other specialties and disciplines as we need to.”
In some states, APRNs must collaborate with a physician for a period or all of the time. And although APRNs can prescribe in all fifty states what they can prescribe can vary from state to state. These practice restrictions have led to calls (including from the National Academy of Medicine, and the National Governors’ Association) to remove all barriers for APRNs to have full practice authority.
A key step in this direction came from the Veteran’s Health Administration’s (VA) rule, finalized in January of 2017, granting full practice autonomy without physician supervision to all VA certified nurse practitioners, certified nurse midwives, and certified clinical nurse specialists when acting within the scope of their VA employment, even in states with reduced or restricted practice.
APRNs are trained under the nursing model, and they bring a holistic perspective that highlights health promotion, disease prevention, health education and counseling, and family involvement. “If you look at it professionally, physicians have historically been trained under the medical model with an emphasis on anatomical structures, physiology and pathophysiology related to disease and health processes,” said Martinez, “whereas, APRNs were trained first within the nursing model with a focus on holistic care and promoting health and well-being by accounting for the whole patient, but then go back and get the advanced practice care education. It is a blending of the two models that makes an APRN.”
Martinez observed that medical education has incorporated a more holistic view with the introduction of humanities and the arts into medical education. “I think as nurses incorporate more of the medical model”, he said, “it appears that medicine is also aligning more with the nursing model.” YSN master’s degree students and Yale School of Medicine (YSM) medical and physician associates (PAs) students are often taught similar material but within the silos of each profession.
This teaching model changed when YSN and YSM collaborated to create the Interprofessional Longitudinal Clinical Experience (ILCE) several years ago. The goal of this innovative course is to help students interact with other healthcare professionals from the very beginning of their training. “Interprofessional training starts a dialogue between two very strong professions, nursing and medicine, and the resulting relationship-building is inculcated in the students,” said Portillo.
During the ILCE, students from each program are teamed up and spend two to four hours every other week for a year seeing patients under the supervision of faculty. “At this point, the students are brand new, and they don’t know what their philosophical differences are,” said Martinez. “It is nice to catch them early and train them from day one to work together to problem solve and think as a team.”
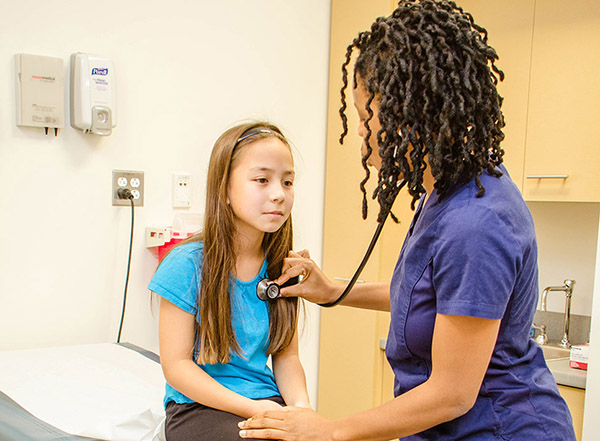
With initial funding from the Josiah Macy Jr. Foundation and The Doctors Company, the ILCE is directed by YSM’s Eve Colson, MD, MEd. “The benefits of interprofessional education are that students learn with, from and about each other,” said Colson. “They understand more about each other’s backgrounds, curricula and capabilities and that helps them a lot when they go into practice. Our next step is to talk about having students meet up again as they are further into their training.”
Equipped with a breadth of clinical training, skills and experiences not all APRNs opt for providing direct patient care. Some go on to careers in administration, research or academia. Luc R. Pelletier, MSN, APRN, PMHCNS-BC, FNAHQ, FAAN, a 1982 YSN master’s graduate in psychiatric-mental health nursing and the recipient of the 2017 Yale School of Nursing Distinguished Alumnae/i Award, has had a diverse career as an APRN. “As a graduate of YSN, I think men bring a richness to the profession,” he said. “My trajectory was administrative and management, research and academics.” An expert in quality healthcare management and an accomplished writer, Pelletier is a Fellow of the National Association for Healthcare Quality, and recently wrote the fourth edition of HQ Solutions: Resource for the Healthcare Quality Professional.
As pressures on the healthcare system intensify, it is anticipated that APRNs will increasingly fill critical roles in providing outstanding patient-centered care. “I’m amazed at the talent out there and how it is contributing to the profession in delivering high-quality care,” Portillo said.
The full article can be seen in the spring, 2018 issue of Yale Nursing Matters, pages 20-23.
